Friday, November 6, 2009
Advanced Spinal Injury Concepts
Frequent readers of my blogs and articles will have read entries concerning disc bulges and herniations and also covering discogenic pain. Those topics concerning the intervertebral discs, along with various traumatic fractures of the spine, make up the vast majority of the spinal injuries involved in litigation. For that reason, most trial attorneys have at least a passing familiarity with these concepts. But there are other issues involving the spine that may be encountered from time to time. These include spondylolisthesis, spondylolysis, spondylosis and ankylosis, and involve different areas of anatomy including the pars interarticularis and the facets. Since these terms are more unusual, fewer attorneys are familiar with these concepts, so today I will provide you with a general overview so that you may be more comfortable when encountering these conditions in future cases.
First, let us begin by discussing the anatomy of the spine. The spine is made up of multiple individual bones called vertebrae that provide support for the weight of the upper body and provide protection for the spinal cord by surrounding it with an armor of bone from the skull all the way down to the pelvis. Each vertebra can be described as a ring with the large cylindrical vertebral body forming the anterior aspect of the ring and the laminae and spinous processes forming the posterior aspect of the ring. The vertebral bodies are aligned with one atop another forming a column providing the majority of the support for the spine. The laminae form a shield protecting the posterior aspect of the spinal cord. It is important to note that the region of the vertebrae where the posterior aspects join with the anterior aspects is called the pars interarticularis. Also there are joints where the posterior elements of each vertebra come together above and below, and these are called facets. Finally, we must understand that the spinal cord branches into nerve roots at each intervertebral level and that these nerve branches exit the spine through channels called foramen that run beneath the facets.
Now that we've covered the pertinent anatomy, let’s discuss the various pathologies that you might encounter when researching a spinal injury. Of course, as mentioned earlier, disc herniations and spinal fractures are the most common injuries you will come across, but there are other conditions you will see from time to time. Spondylolisthesis, sometimes referred to as anterolisthesis, is a defect in the alignment of the vertebral bodies allowing one vertebral body to slip forward over the vertebral body at the level beneath. In most cases the entire spine, above the level of the defect, is displaced anteriorly. In other words, if you have a spondylolisthesis at L5-S1, the L5 vertebral body will be displaced forward in relation to the sacrum (S1) but L5 will still maintain its proper alignment with L4 and the other vertebrae above. While it may be easy to imagine this change in relationship between the vertebral bodies, it is more difficult to visualize the changes in the posterior aspect of the spine that allow this displacement to occur. In order for the vertebra to move forward the posterior articulations at the facets must be either dislocated or weakened, or there must be a separation in the pars interarticularis (another condition called spondylolysis) allowing for a separation of the vertebra itself. While such a defect in the pars is generally a congenital or pre-existing condition, trauma can cause a worsening of the actual displacement resulting in the spondylolisthesis that is eventually diagnosed. Spondylolishesis is a problem because it can change the passageway for the spinal cord down through the spinal canal causing compression or stretching of the spinal nerves. It can also place tension of the exiting nerve roots at the specific level of displacement or may be associated with a disc herniation at the level of instability. Spondylolisthesis can be mild to severe and if symptomatic is generally treated with a spinal fusion procedure including bone grafts and fusion hardware.
The final pathology we will discuss is spondylosis (sometimes referred to as ankylosis). Basically, this is simply arthritis of the spine. This arthritis may develop over time following the trauma involved in a case, or it may be preexisting and exacerbated by the injury of your case. As with all forms of arthritis, spondylosis primarily affects the joint surfaces. This can include the endplates of the vertebral bodies adjacent to the discs in the anterior aspect of the spine, or the articular surfaces of the facet joints in the posterior aspect of the spine. As with other forms of arthritis, this condition can cause localized pain within the joints themselves or can cause overgrowths of bone (bone spurs or osteophytes) that can protrude into vital regions causing compressions of vulnerable nerves including the spinal cord and nerve roots. As we learned earlier, the foramen through which the nerve roots travel are adjacent to the facets, so overgrowth of arthritis in this area can narrow these foramen and impinge upon the nerve roots. Spondylosis can be treated with a variety of procedures ranging from simple steroid injections to widespread spinal fusion surgery, based on the severity of the condition. The key issue is to remember that although this is an arthritic condition, it can be still linked specifically to trauma.
Monday, October 5, 2009
Classification of Burns

How do you classify burn injuries? At one time, this was a fairly simple question to answer, but the classification of burns is changing and a new system is gradually being adopted. This has made conversations about burns more complicated since you need to be sure that everyone concerned is using the same system and terms. This article will cover the basics and discuss terminology that you might face when handling your next burn injury case.
Traditionally, burns have been categorized as first-, second-, or
 third-degree. This system is defined by the following categories:
third-degree. This system is defined by the following categories:• First-degree burns affect only the epidermis, or outer layer of
skin. The burn site is red, painful, dry, and with no blisters. Mild sunburn is an example.
• Second-degree burns involve the epidermis and part of the dermis
 layer of skin. The burn site appears red, blistered, and may be swollen and painful.
layer of skin. The burn site appears red, blistered, and may be swollen and painful.• Third-degree burns may also damage the underlying bones, muscles, and tendons. The burn site appears white or charred. There is no sensation in the area since the nerve endings are destroyed.
For many years, healthcare providers have also added a fourth-degree
 category. Using this system, third-degree burns are limited to those that extend down through the epidermis and dermis into the subcutaneous tissue, and fourth-degree describes the burns that extend down into the underlying muscles, tendons and ligaments.
category. Using this system, third-degree burns are limited to those that extend down through the epidermis and dermis into the subcutaneous tissue, and fourth-degree describes the burns that extend down into the underlying muscles, tendons and ligaments.Recently, a new system has come into use. This new system completely abandons the old use of degrees and describes the injuries based specifically by the depth of the burn. The traditional classification of burns is being replaced by the designations of superficial, superficial partial thickness, deep partial thickness and full thickness. Of course, these designations refer to the depth of the skin affected by the burn.
For now, the change in systems is still in progress, so during the transition you will notice a blend of terminology. Some experts may refer to first-degree, second-degree, third-degree and full thickness burns. Some may use a combination of terms such as first-degree/superficial, second-degree/partial thickness, third-degree/deep partial thickness and fourth-degree/full thickness. The variations can become confusing, so it is good to be versed in all the terms and systems discussed above.
Monday, August 31, 2009
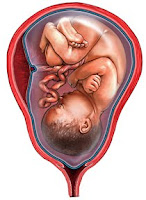
Variations in Fetal Orientation During Pregnancy
Obstetrics litigation often boils down to a question of what events occurred within the uterus during development or during the birthing process. Often, if we are to understand what happened to the fetus at a crucial moment in the pregnancy, we need to have a clear understanding of how that fetus is positioned within the uterus or the birth canal. For this reason, issues of fetal lie, presentation, position or station are eventually discussed in almost all obstetrics cases. Therefore, I will try to provide you with a basic understanding of these concepts so that you can better visualize the wide variety of ways that the baby can be positioned within the mother.
First of all we have to establish our terms. For the purposes of this conversation, I’d like for you to visualize the mother in a standing position so that “down” is toward her feet and “up” is toward her
 head. “Posterior” is toward her back and “anterior” is toward her front. Right will always mean her right regardless of how the baby is positioned or how you are standing. Just remember that when I use directional terms, it’s all about the mother.
head. “Posterior” is toward her back and “anterior” is toward her front. Right will always mean her right regardless of how the baby is positioned or how you are standing. Just remember that when I use directional terms, it’s all about the mother.Keep in mind that it is of paramount importance to know the orientation of the fetus within the uterus, particularly at the onset of labor. Orientations that are not ideal may require intervention and, in some situations, cesarean delivery may be the only viable option. During labor, an appreciation of the fetal station within the birth canal can help us to judge how the labor is progressing and which delivery techniques may be warranted at a given time.
Traditionally, the orientation of the fetus is described with respect to its lie, presentation and position. I will provide an overview of these terms. The lie of the fetus can be either longitudinal or transverse. In other words, the long axis of the fetus can either be parallel or perpendicular to the long axis of the mother. Luckily, the fetal lie is longitudinal in about 99% of cases. This is a good thing since a transverse lie cannot allow for the proper vaginal delivery of the fetus.
Once we know the lie, we can determine the presentation. The presentation can be either cephalic or breech, which means that the fetus can be either “head-down” or not. There are a number of different types of cephalic presentation, but the most common is called vertex presentation which refers to the fetus entering the birth canal head first with the upper occipital (back) portion of the head leading the way.
Next, the position of the fetus can be established. Position refers to the relation of the occiput (back of the skull) of the fetus to the
 left, right, front and back of the mother. In other words, if we know that the back of the fetal head is facing the front of the mother, this is called the occiput anterior (OA) position and if the occiput is facing the right side of the mother, this is called the right occiput transverse (ROT) position. Any combination of these, where the occiput of the fetus is toward the right and toward the front in a diagonal fashion, is called the right occiput anterior (ROA) position. This convention allows us to note any one of the following eight positions: occiput anterior (OA), right occiput anterior (ROA), right occiput transverse (ROT), occiput posterior (OP), left occiput posterior (LOP), left occiput transverse (LOT), and left occiput anterior (LOA).
left, right, front and back of the mother. In other words, if we know that the back of the fetal head is facing the front of the mother, this is called the occiput anterior (OA) position and if the occiput is facing the right side of the mother, this is called the right occiput transverse (ROT) position. Any combination of these, where the occiput of the fetus is toward the right and toward the front in a diagonal fashion, is called the right occiput anterior (ROA) position. This convention allows us to note any one of the following eight positions: occiput anterior (OA), right occiput anterior (ROA), right occiput transverse (ROT), occiput posterior (OP), left occiput posterior (LOP), left occiput transverse (LOT), and left occiput anterior (LOA).Finally, we can discuss fetal station. The fetal station is a measurement of how far the fetus has progressed down through the birth canal during delivery. This measurement reflects the relationship of
 the leading edge of the fetus, generally the top of the head, to the ischial spines of the mother’s pelvis that are halfway between the pelvic inlet and pelvic outlet. When the leading edge of the fetus reaches the ischial spines, this is called zero (0) station. In the currently used “fifths” system the space is divided above and below 0 station in one centimeter increments, so that the space above the ischial spines is designated from -5 station to 0 station and the space below the ischial spines is designated from 0 station down to +5 station. With each centimeter that the leading edge of the fetus progresses, you reach a new station of presentation (-5, -4, -3, -2, -1, 0, +1, +2, +3, +4, +5).
the leading edge of the fetus, generally the top of the head, to the ischial spines of the mother’s pelvis that are halfway between the pelvic inlet and pelvic outlet. When the leading edge of the fetus reaches the ischial spines, this is called zero (0) station. In the currently used “fifths” system the space is divided above and below 0 station in one centimeter increments, so that the space above the ischial spines is designated from -5 station to 0 station and the space below the ischial spines is designated from 0 station down to +5 station. With each centimeter that the leading edge of the fetus progresses, you reach a new station of presentation (-5, -4, -3, -2, -1, 0, +1, +2, +3, +4, +5). You should be aware that a previously widespread system, the “thirds” system, divided the space above and below the ischial spines into arbitrary thirds so that the stations progressed from -3 to +3 without regard to actual centimeter measurements. This is important because only 0 station coincides in these two systems and you can get an inaccurate picture of the case facts if the correct system is not used. To complicate matters, many doctors and hospitals still refer to the old system so it is best to establish early which system is being used in the records of any particular case.
These are the key terms that you will encounter when researching almost any case involving birth injuries or obstetrics mal practice. Hopefully this overview has given you a better understanding of the varieties of fetal orientation and will help you to better visualize the lie, presentation and position of the fetus within the womb.
Tuesday, August 11, 2009
Nursing Home Negligence Cases
One of the most common nursing negligence issues we are called upon to illustrate is the development or progression of pressure sores (sometimes know as bed sores or decubitus ulcers). Pressure sores are areas of injured skin and tissue usually caused by sitting or lying in one position for too long. This often happens if you use a wheelchair or you are bedridden, even for a short period of time (for example, after surgery or an injury). When a change in position doesn't occur
.jpg) often enough and the blood supply gets too low, a sore may form. The constant pressure against the skin reduces the blood supply to that area, and the affected tissue dies.
often enough and the blood supply gets too low, a sore may form. The constant pressure against the skin reduces the blood supply to that area, and the affected tissue dies.A pressure sore starts as reddened skin but gets progressively worse, forming a blister, then an open sore, and finally a crater. The most common places for pressure sores are over bony prominences (bones close to the skin) like the elbow, heels, hips, ankles, shoulders, back, and the back of the head. Pressure sores are categorized by severity, from Stage I (earliest signs) to Stage IV (worst):
• Stage I: A reddened area on the skin that, when pressed, is "non-blanchable" (does not turn white). This indicates that a pressure ulcer is starting to develop.
• Stage II: The skin blisters or forms an open sore. The area around the sore may be red and irritated.
• Stage III: The skin breakdown now looks like a crater where there is damage to the tissue below the skin.
• Stage IV: The pressure ulcer has become so deep that there is damage to the muscle and bone, and sometimes tendons and joints.
In most cases pressure sores are preventable and, if not prevented,
.jpg) should be recognized early and appropriately treated. In almost all situations, the development of massive pressure sores is evidence of some form of deviation in the standard of nursing care (neglect). Generally the neglect is in more than one area, i.e., hygiene, nutrition, infection control, protection and positioning.
should be recognized early and appropriately treated. In almost all situations, the development of massive pressure sores is evidence of some form of deviation in the standard of nursing care (neglect). Generally the neglect is in more than one area, i.e., hygiene, nutrition, infection control, protection and positioning.The common areas for the formation of pressure sores and their prevention is a basic area covered in all nursing schools by all licensed nursing programs (LVN or RN). Prevention consists of changing the person's position every two hours or more often if needed. The two-hour time frame is a generally accepted maximum interval that tissue can tolerate pressure without damage. Prevention also consists of protection and padding to prevent tissue abrasion as well as the elements of nutrition, hydration, hygiene, etc. Turning and positioning is common knowledge for physicians, licensed nurses (LVN or RN), and physical therapists as well as paraprofessional care gives (nursing assistants). Turning is applicable even on flotation mattress beds.
Treatment for pressure sores involves removing all pressure from the involved area(s) to prevent further decay of tissue and promote healing. Frequent turning is mandatory to alleviate pressure on the wound and to promote healing. Treatment also involves keeping the area clean, promoting tissue regeneration and removing necrotic (dead)
.jpg) tissue, which can form a breeding ground for infection. There are many procedures and products available for wound care, cleaning and pressure reduction. The use of antibiotics when appropriate is also part of the treatment. Some deep wounds even require surgical removal or debridement of dead tissue. Without all of these elements being in place, the wounds will not heal and, in fact, will quickly worsen.
tissue, which can form a breeding ground for infection. There are many procedures and products available for wound care, cleaning and pressure reduction. The use of antibiotics when appropriate is also part of the treatment. Some deep wounds even require surgical removal or debridement of dead tissue. Without all of these elements being in place, the wounds will not heal and, in fact, will quickly worsen.
Friday, July 17, 2009
Linking the Evidence of Traumatic Brain Injury
Brain injuries are one of the most common topics involved in personal injury litigation. Motor vehicle collisions, falls, sports injuries and many other circumstances with associated impacts frequently damage the brain, the most important and vulnerable organ in the body. The severity of these injuries can range from mild to severe. Cases may or may not involve surgery or other medical interventions. But in almost all brain injury cases, there exist similar challenges for selecting or crafting demonstrative evidence.
In traumatic brain injury cases, you will most likely have significant
 radiological evidence. Hematomas, contusions, and areas of infarction, etc. typically show up nicely on CT or MRI studies. You may choose to simply utilize these radiological studies as your demonstrative evidence. While this is certainly the most affordable option, you should consider having a skilled medical illustrator either highlight these films, coloring the pertinent regions, or have the illustrator create full color illustrations interpreting the films in greater detail. These are generally some of the most affordable custom
radiological evidence. Hematomas, contusions, and areas of infarction, etc. typically show up nicely on CT or MRI studies. You may choose to simply utilize these radiological studies as your demonstrative evidence. While this is certainly the most affordable option, you should consider having a skilled medical illustrator either highlight these films, coloring the pertinent regions, or have the illustrator create full color illustrations interpreting the films in greater detail. These are generally some of the most affordable custom  exhibits you could purchase, but they certainly make a big difference in clarifying the injuries for the layperson.
exhibits you could purchase, but they certainly make a big difference in clarifying the injuries for the layperson.Your next most valuable bit of evidence may be the neurological evaluation. This report will detail the neurological deficits or behavioral changes experienced by the patient following the injury. This report in itself is a valuable tool, but it can be even more effective if you can create a direct link between the radiological evidence and the neurological evaluation. For example, if your neurological evaluation discusses significant changes in the patient's short-term memory and balance and we can clearly see a physical injury on the radiological studies that affects the temporal lobe, then we have an opportunity for the foundation of a great argument linking these factors. Since the temporal lobe is damaged and the temporal lobe is responsible for the symptoms experienced by the patient we must create a visual link for the jury so that there is no doubt that the two reports are related. It doesn't matter if you employ a simple chart mapping brain functions or a complex presentation concentrating
 on your specific area of interest. The goal is to establish a foundation of knowledge in the viewer so that the links between cause and effect can be appreciated.
on your specific area of interest. The goal is to establish a foundation of knowledge in the viewer so that the links between cause and effect can be appreciated.For any neurological evaluation, you should take the extra time to inquire from the neurologist, not only what deficits can be seen, but also what regions of the brain influence the pertinent brain functions. After the region of functional deficit is determined, you can go back to the original diagnostic radiological studies to see if the visible injury is in the same region. The brain is complex, so you may not always have a direct match, but in those cases where the two reports coincide, you would be well served to take the time to educate your audience on the functional regions of the brain. This way a direct link can be drawn between the injury and the subsequent neurological symptoms.
Of course, there are many other types of demonstrative evidence that can be useful in these traumatic brain cases including dramatic illustrations of brain surgery or mechanism of injury animations. Perhaps that will be a topic for another day.
Monday, June 29, 2009
Discogenic Spine Pain
When I started in this industry, almost 20 years ago, my very first case involved a lumbar disc injury with a subsequent discectomy and fusion surgery. Since that first case, I've probably worked on hundreds if not thousands of similar cases. Any medical illustrator who works for attorneys will probably agree that intervertebral disc cases are the most common projects we receive. If you've been handling personal injury or medical malpractice cases for a while you've probably seen more than a few disc cases yourself.
Thankfully, new developments in the sciences of disc injury and surgical techniques have kept this topic from getting stale. Where once we saw fixation accomplished with things like Harrington rods or Cotrel-Debousset instrumentation that could easily be confused with medieval torture devices, we now see pedicle screw fusion hardware, and even percutaneous discectomy procedures that do not require large open incisions. While once there were only different shapes of harvested bone grafts, there is now a variety of titanium and synthetic cages or spacers that can be employed to replace an offending disc.
Today, I'd like to discuss spinal discogenic pain. Discogenic pain is pain that comes from the disc itself. Although some medical experts have been discussing the issue for years, it is a fairly groundbreaking concept that is relatively new in our industry. This is not just the standard discussion of disc bulges and disc herniations that can compress the adjacent nerves, but rather a discussion of the pain that comes from the disc itself when it is damaged.

Traditionally, many experts discounted intervertebral disc cases that showed clear evidence of disc injury if there was not also evidence of spinal cord or nerve root compression. Their rationale was that nerves generate and transmit pain, therefore if there is no compression of a nerve then there can not be real pain. However, it is now becoming clear that there are at least two ways that pain can originate from an injured disc that does not involve direct compression of the spinal cord or nerve roots.
The first mechanism of discogenic pain involves the recurrent meningeal nerves. These nerves branches off of the ventral rami of the nerve roots outside of the spinal canal and then course back in through the neural foramen to innervate the posterior annulus of the discs as well as the posterior longitudinal ligament. These nerves sense when the annulus or posterior longitudinal ligament is stretched, strained or torn. Nerve impulses then flow through the recurrent meningeal nerve, through the nerve root, up the spinal cord
 and into the brain to stimulate the pain centers. Injuries to the discs are no different than injuries to the fingers, toes or any other part of the body. Pain originates wherever there are nerves to transmit sensory impulses from damaged tissue.
and into the brain to stimulate the pain centers. Injuries to the discs are no different than injuries to the fingers, toes or any other part of the body. Pain originates wherever there are nerves to transmit sensory impulses from damaged tissue.The second mechanism discussed in recent literature concerns the caustic effects of the fluid normally contained within an intervertebral disc. When the annulus of the disc is torn, fluid from within the disc may leak out into the spinal canal (passageway of spinal cord) or neural foramen (passageway of nerve roots). This fluid contains inflammatory cytokines, chemicals that have an inflammatory effect. Inflammatory cytokines act as a strong irritant causing severe inflammation and pain. Recent studies on rats show that chemicals extracted from the nucleus of a damaged intervertebral disc which results in the rat walking with a limp, implying that the rat is experiencing pain.

Also, when these chemicals come into contact with a nerve root, it can cause typical radiculopathy, paresthesia, weakness, and sensory and motor loss symptoms even though the MRI may show no nerve root impingent at all. It is believed that this inflammation is helpful in the reabsorption and healing of a herniated disc, but these same chemicals can have a harmful effect on the adjacent nerve roots. This is one explanation why a patient who's herniation may appear to have
 healed on a subsequent MRI may still be experiencing significant symptoms.
healed on a subsequent MRI may still be experiencing significant symptoms.I mention all this as a means of illustrating that new science is constantly bringing forth new questions and new answers in all areas, even those we think we have seen a thousand times before. It is vital that we continue to keep abreast of new theories and new discoveries to be sure that we are utilizing the best tools at hand to understand the subtleties of the issues in each case. I will continue to try to keep you informed of some of these issues through this forum in the weeks and months ahead.
Monday, June 15, 2009
Anatomy of the Shoulder and Rotator Cuff

I have received an inordinate number of calls this week from attorneys with rotator cuff injury cases or medical malpractice cases involving arthroscopic shoulder repairs. Regretfully, many of these conversations have reinforced my opinion that the shoulder is one of the most widely misunderstood areas of anatomy that is frequently involved in litigation. To many attorneys this ball and socket joint seems like a confusing mass of tendons and skeletal structures with functions that are difficult to recognize and names that are hard to pronounce. It certainly doesn’t need to be that hard. I’ll take just a few minutes to provide a basic overview of the anatomy of the shoulder so that you’ll be better prepared in your next personal injury or medial malpractice case.

In my opinion, the key to understanding the entire shoulder is a thorough understanding of the scapula (shoulder blade). The scapula is a fairly flat triangular shaped bone located on the upper outer portion of the back. The back of the scapula is divided by a ridge called the spine that we will be important to remember later when we discuss the rotator cuff. You should also note the two small projections or processes that protrude from the scapula. The tip of the spine becomes the acromion process projecting upward which articulates with the clavicle (collar bone). Also there is the coracoid process that projects forward.
 Both of these processes provide attachments to various muscles of the chest and arm. The final skeletal aspect of the scapula that you need to appreciate is the glenoid cavity that forms the socket portion of the ball and socket joint of the shoulder.
Both of these processes provide attachments to various muscles of the chest and arm. The final skeletal aspect of the scapula that you need to appreciate is the glenoid cavity that forms the socket portion of the ball and socket joint of the shoulder.The rotator cuff is a group of four muscles that that extend from the scapula to the humerus (upper arm bone) to provide stability and prevent dislocation. The first three of these muscles are named in association with where they lie in relation to the scapula. Now that you appreciate the skeletal anatomy of the scapula, you will better understand these names. The supraspinatus runs along the top of the scapula above the spine. The infraspinatus runs along the back of the scapula beneath the spine. The subscapularis runs beneath the scapula. There is also the teres minor which runs on the back of the scapula at the very bottom. Any or all of these muscles or the tendons that connect them to the humerus can be injured, but in my experience, the supraspinatus is by far the most commonly injured. One reason for the vulnerability of the supraspinatus is that it runs beneath the acromioclavicular joint where the clavicle joins the acromion process. Injury to either surface of this joint can cause bone spurs that protrude down leading to tearing of the underlying supraspinatus tendon.
Of course there are other aspects of the shoulder that I haven’t discussed here such as the glenoid labrum, the subacromial bursa, the vessels of the thoracic outlet or the nerves of the brachial plexus. Perhaps we will return to the shoulder in future articles and explore this wonderfully complex joint in greater detail.
Subscribe to:
Posts (Atom)
